Structured Agenda-free Coaching Conversations (“StACC”)
Structured Agenda-free Coaching Conversations (StACC) - Building patient capability beyond clinical treatment
What is the StACC model?
The StACC Model is an evidence-based coaching approach designed to increase activation, support self-management and, as a result, improve an individual’s health and wellbeing outcomes while reducing unnecessary reliance on clinical and other public sector services.
While often used for the management of long-term health conditions, target outcomes can relate to any aspect of a person’s life, including physical health, mental health, general wellbeing, lifestyle changes, employment, education, and personal circumstances.
It is a structured, replicable methodology that enables individuals to:
identify what’s important to them right now
take meaningful, achievable action
build their knowledge, skills, and confidence to self-manage effectively
internalise the process and use it to address further challenges or goals
How is the StACC Model used?
The StACC Model can be used in two primary ways:
1. As a dedicated, stand-alone intervention
Delivered over a series of sessions (typically 5–8), where supported self-management (SSM) and increased activation are being used as a means to improve outcomes. ‘Health and Wellbeing Coaches’ were introduced into NHS Primary Care in 2020 for this purpose.
2. Integrated within existing support roles
Embedded into any role that provides structured, multi-session support.
While these roles often have specific, defined objectives, incorporating the StACC model into the role can greatly enhance outcomes.
This includes roles such as:
Community Connectors
WorkWell Coaches
School pastoral support staff
Care Coordinators
Social Prescribing Link Workers
Various health, mental health or social care roles
Statutory sector roles (e.g. employment or education services)
Community and voluntary sector workers
Public or private sector workforce support roles
Any multi-session support role focused on improving an individual’s health or wellbeing in any way
Wider application
The StACC skillset can also be applied more broadly by anyone wishing to use supported self-management skills within their role. This may include doctors, teachers, parents, managers, and anyone in a role where they are supporting others.
How Does the StACC Model Work?
The model works by establishing ownership and engagement first, before moving to action to support the building of confidence and problem-solving skills.
While this sequence is essential, coaches nonetheless flex backwards and forwards within the structure as necessary to ensure they are meeting patients where they are at all times and then supporting them to move forward.
As the individual is being guided through a process, the process is able to be internalised by the individual and applied to further challenges and goals, supporting sustained behaviour change and long-term self-management.
Read more in ‘Evolution of the StACC model’ and ‘How StACC works to increase activation’, below
Why is StACC’s focus on ownership and engagement important in the context of supporting self-management and increasing patient activation?
StACC’s initial focus on ownership and engagement, before moving to action, addresses two key factors in the literature for the management of long-term conditions that are sometimes overlooked.
‘Ownership’ and the Wanless Review (2002)
The Wanless Review (2002): Securing our future health: Taking a long‑term viewhighlighted the central role that ‘ownership’ plays in how well people manage their health and wellbeing. The Report describes how:
“Public health improves dramatically with a sharp decline in key risk factors such as smoking and obesity, as people actively take ownership of their own health.”
This ‘fully-engaged scenario’, as Wanless called it, was also shown to be the least expensive scenario for the NHS, providing estimated savings to the NHS of up to £30 billion in resource needs by 2022.
A Roundtable discussion “Ten Years on from Wanless” held in 2012 highlighted how the fully-engaged scenario had so far not been met as “we still have a paternalistic service and a dependent population”.
Supporting patients to take ownership helps to move patients from passive recipients of healthcare to active participants in their health and wellbeing.
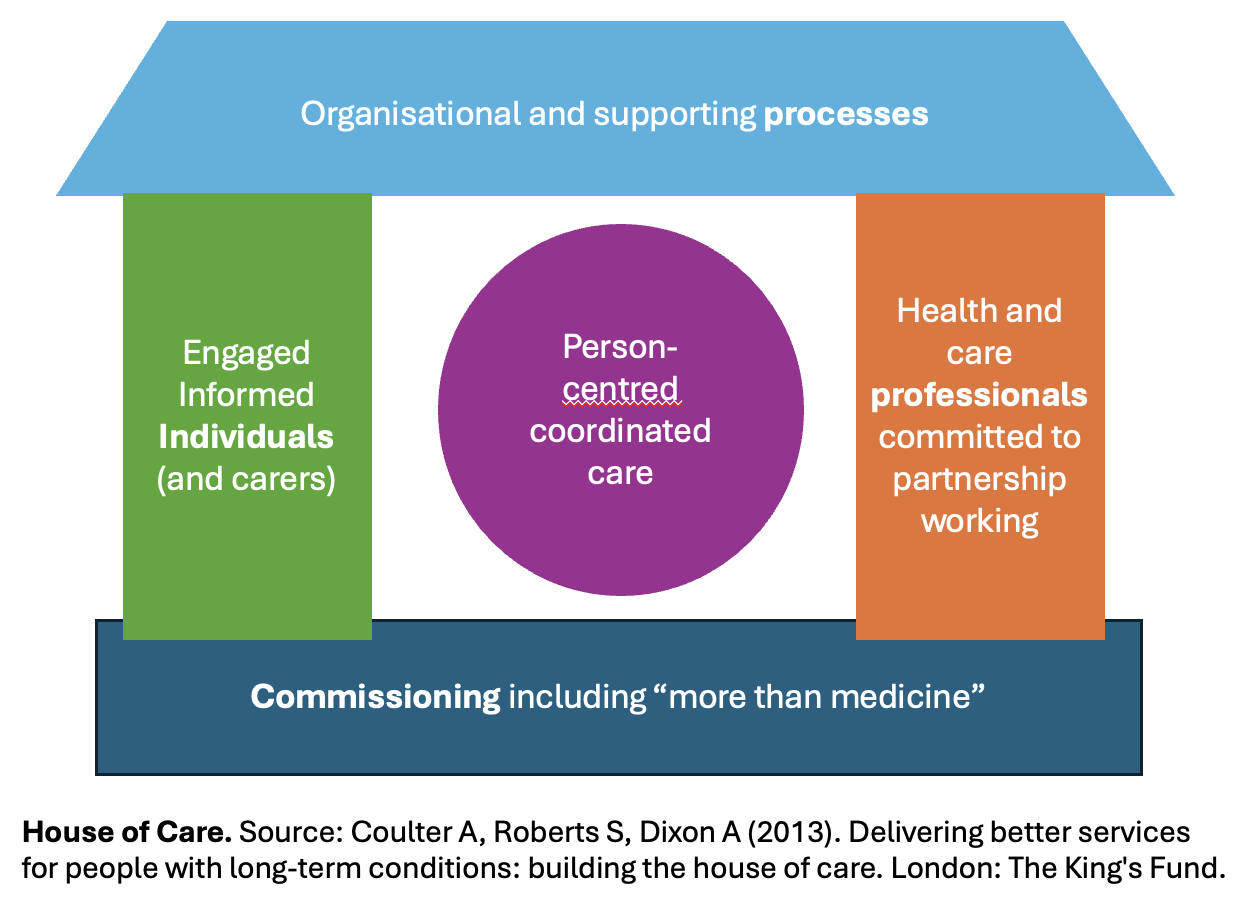
Engaged, Informed Patients and the House of Care
The House of Care framework is widely used in the NHS to guide the management of long-term conditions.
The “right-hand wall” represents “health and care professionals committed to partnership working [with patients]”. Training in Shared Decision Making is designed to support Clinicians in this aim.
The “left-hand wall” represents the the role of ‘engaged, informed patients’, acknowledging that effective management of long-term conditions relies in part on patients being active participants in the management of their health and wellbeing.
However, if patients are not engaged and are not supported to become engaged, they are unable to fulfil their part of this framework, and the potential benefits of coordinated care may not be realised.
StACC’s focus on ownership and engagement addresses this potential weakness, thereby strengthening the effectiveness of the House of Care framework.
Where did the StACC Model come from?
The Evolution of the StACC ModelThe StACC model is the product of over three decades of development in self‑management support, patient activation research, and coaching practice.
Its evolution reflects learning from established group‑based self‑management education programmes, refinements in coaching and behaviour change practice, and systematic integration with patient activation theory.
The timeline below traces this evolution from the early self‑management work in the USA as an health condition issue-based peer-led group intervention through to the current StACC model as used in NHS and personalised care settings as a one-to-one non-condition- and non-issue-based intervention delivered by trained coaches and aimed at increasing activation as a way to support people to build their knowledge, skills and confidence to self-manage effectively.
-
The Chronic Disease Self-Management Programme - also known as “The Stanford Model” - is a 6-week peer led group programme developed by Dr Kate Lorig and her team at Stanford University in the early 1990’s to support people in managing various issues commonly associated with the management of long term conditions, such as fatigue, low mood, etc. A scale measuring people’s confidence to manage long-term conditions, the Chronic Disease Self-Efficacy Scale, was developed by Lorig et al in 1996.
-
The Stanford Model was introduced in the UK as ‘The Expert Patient Programme (EPP)’ by the Department of Health in 2002. It followed the same format of being a 6-week peer-led group programme focused on issues commonly facing people managing one or more long-term conditions.
-
Hibbard et al (University of Oregon) described a process for conceptualising what it means to be ‘activated’ in the self-management of long-term conditions and created the Patient Activation Measure (‘PAM’), a 13-point questionnaire designed to assess an individual’s level of ‘active’ engagement in the management of their health.
-
The Health Foundation’s Co-creating Health Programme was a whole-system programme designed to embed supported self-management within NHS services for people with long-term conditions. It involved three pillars: patient self-management, clinician training, and system change. The Self-Management Programme (for patient self-management) used three Coaching Conversation steps from EPP: Agenda-setting, Eliciting the Story, and Goal-Setting. By the end of the programme, two further steps from Motivational Interviewing had been added: Establishing Importance and Goal Follow-up. This 5-step model emerged from the programme as a model informally named ‘The Coaching Conversation Flow’.
-
Know Your Own Health worked with founding members of EPP, including the National Support Lead for the Co-Creating Health Self-Management Programme, supporting and delivering one-to-one coaching using the Coaching Conversation Flow. Through collecting outcomes data using various patient activation measurements including the PAM, it became clear that the Coaching Conversation Flow could be used in two ways to support self-management. The model as used in the Co-Creating SMP Health Programme demonstrated increases in activation of around 8 points. Alternatively, used an agenda-free intervention aimed at supporting patients to take ownership and build their confidence and problem-solving skills, the model showed increases in activation of around 14 points together with associated improvements in self-management, improved outcomes and reduced reliance on health services.
-
Training in the PCI Core Curriculum Health Coaching Skills together with the StACC Model accredited as:
a 4-day training for Health and Wellbeing Coaches and others delivering coaching as an intervention in any context
a 2-day training in the toolkit of skills and an introduction to the model
-
How StACC works with patient activation levels

The steps of the StACC model reflect the patient activation levels as delineated by Hibbard et al in 2004 (See References in Background). Depending where someone starts in terms of activation or how stuck they are feeling will dictate the pace with which they move and/or flex through the steps - taking ownership and control before taking action and building confidence and problem-solving skills.